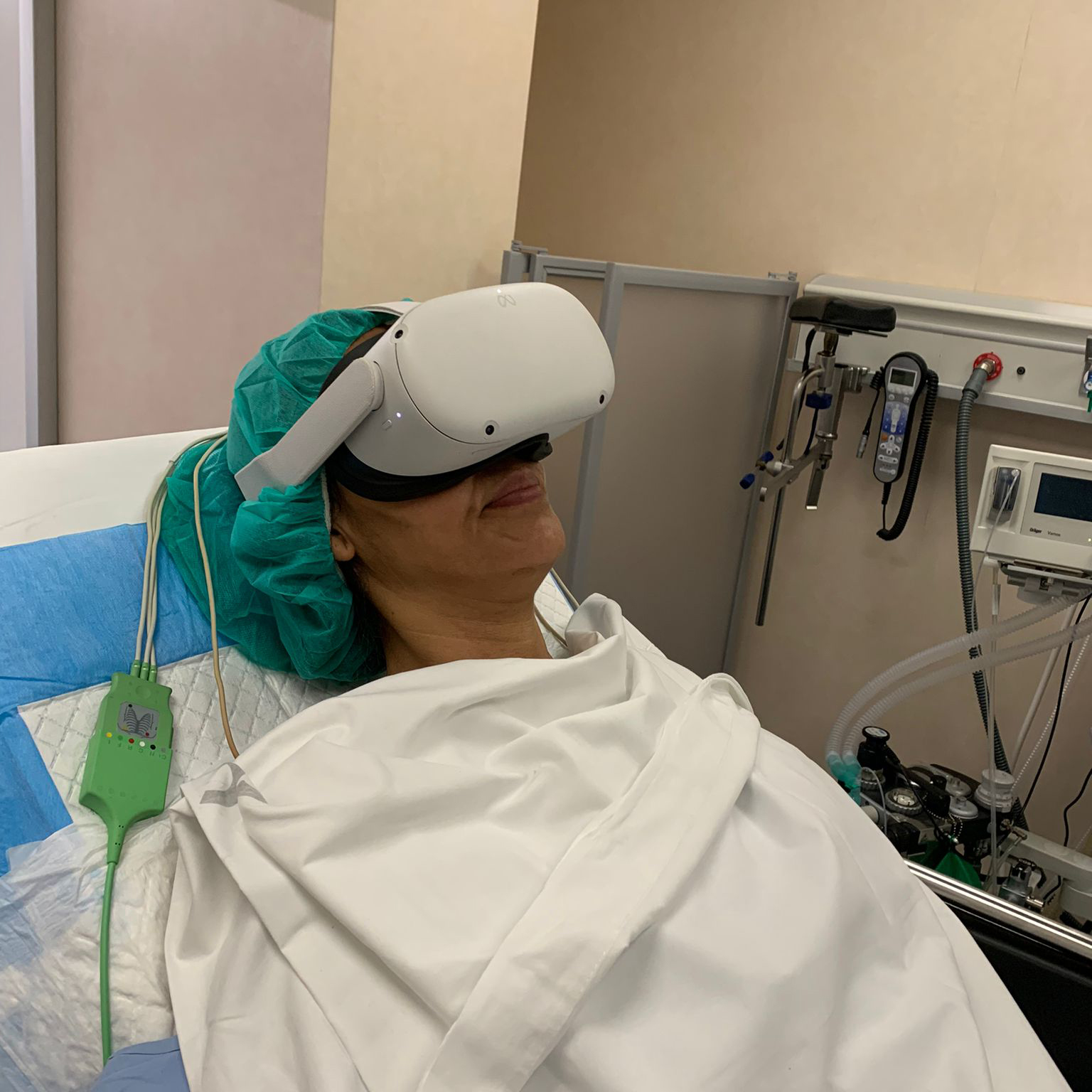
Maria (fictional name) has a scheduled surgical intervention to remove a malignant tumour from one of her breasts. She is the pre-op room, waiting to go into the OR, where the surgery will be performed under general anaesthetics. No wonder she feels anxious, her heart beats very fast, and she is unable to think about anything else right now. Her blood pressure is also going up.
A doctor approaches and, as previously agreed with her, slightly alters the inclination of the gurney Maria is lying on, so that she is now in a half sitting position. He then fits her with virtual reality goggles. For eight minutes, she is going to see a natural landscape and hear relaxing sounds, as a voice guides her meditation in Portuguese.
Before this, Maria performed a first self-assessment of her nervousness by filling out a very simple questionnaire about her level of anxiety and well-being in the imminence of the surgery. She will again answer the same questions in eight minutes, after her experience with meditation in virtual reality settings ends and her goggles are removed.
Later, in the recovery room, Maria will have to answer the questionnaire yet one more time, and if she so wishes, describe how she feels in free text form. Meanwhile, her blood pressure and cardiac rhythm will have been measured and registered at the beginning of the procedure, four minutes into it and at the end, eight minutes afterward.
Maria is one of the 90 patients who agreed to participate in a trial that is going to be launched at the end of the year by a group of surgeons of the Champalimaud Foundation’s Breast Unit, and which aims at evaluating the benefits of combining meditation with virtual reality to relieve the pre-operative stress of patients like her – that is, of women who, having been diagnosed with breast cancer, need surgery with general anaesthetics to treat their disease.
The trial will be presented on May 5, 2023, by David Pinto, one of surgeons in charge of it, during the congress Breast Cancer Metaverse, which will take place at the Champalimaud Foundation and is organised by the AECIMA (the Spanish Association of Breast Surgeons). The other Breast Unit surgeons also in charge of the trial are Pedro Gouveia, Rogélio Andrés-Luna and Maria João Cardoso. Also collaborating in the project are Luzia Travado (psycho-oncologist), OR nurses and anaesthesiologists, neuroscientists Scott Rennie and Razvan Sandru (from the Systems Neuroscience Lab at Champalimaud Research), and Rita Tinoco, who represents the patients.
“It is not uncommon for patients awaiting surgery to feel anxious, and time [spent] in the pre-operative room is described by patients as being (...) most stressful and unpleasant”, states the presentation of the trial. “(...) and there is growing evidence that [virtual reality] meditation could be even more effective than conventional techniques.”
The researchers will consider the results of the trial as positive if the reduction in anxiety and the mood improvement experienced by the patients are greater than two levels; and if the cardiac rhythm and average blood pressure of the patients, as they enter the OR, are decreased by more than 10%.
This clinical trial of so-called “immersive guided meditation”, has been dubbed FLOW, after the name of the VR meditation software that will be used within the virtual reality goggles. The FLOW VR app was developed by a team in Iceland led by Tristan Gribbin, the founder of Flow (www.flow.is). Gribbin is a North American software developer and meditation specialist living in Iceland.
The use of virtual reality as a “distraction manoeuvre” during medical procedures has been described in the literature, with benefits for pain and distress control. But, says Andrés-Luna, “as far as we know, there is nothing in the literature about meditation applied to health with virtual reality in a surgical context.”
To compare different protocols, the participants will randomly be assigned to one of three groups. In one of the groups, the patients will not have virtual reality goggles, nor hear sound or guided meditation. In another, they will be fitted with virtual reality goggles and will see a natural landscape and hear sound, but not the guided meditation voice. Lastly, the patients in the remaining group will be fitted with virtual reality goggles, see a landscape and hear sounds – and the guided meditation voice.
During the eight minutes of the virtual reality experience, an electroencephalogram will also be registered, to allow for calculating their so-called BIS (bispectral index) in order to assess each patient's level of consciousness. The scientists want to be able, by doing this, to determine the impact of the immersive guided meditation experience before patients are sedated.
They also intend, as a next step, to widen the scope of the trial by including patients submitted to surgery with local anaesthetics and to chemotherapy.
Text by Ana Gerschenfeld, Health & Science Writer of the Champalimaud Foundation.