- Clinical Areas
Multidisciplinary Pathology Units
Digestive Unit
The Digestive Cancer Multidisciplinary Unit of the Champalimaud Clinical Centre was created in the last quarter of 2013, under the leadership of oncologist, Dr. Carlos Carvalho. It covers the diagnosis and treatment of digestive tract, liver, bile duct and pancreatic tumours and sarcoma.
The Digestive Unit is composed of two sub-units: the Colorectal Cancer (colon, rectum) and the cancer of the Liver, Bile Duct and Pancreas (HPB); Esophagus and Stomach; Sarcoma; Peritoneal Disease (Cytoreductive surgery and HIPEC) and Thyroid.
Digestive Unit
Colorectal Cancer Programme
A strong commitment
The Colorectal Cancer Group of the Digestive Unit of the Champalimaud Clinical Centre focuses on cancer and the propensity to develop cancers of the digestive tract, including the neuroendocrine system. This group comprises medical oncologists, gastroenterologists, surgeons, radiotherapists and specialised nursing personnel. The Unit utilises a multidisciplinary approach and makes use of the most advanced techniques to deal with the complexity of digestive tumours in all their forms and levels of development. This working group is focused on mastering the knowledge and the intervention techniques in order to halt or delay the development of colorectal cancer, which is currently the second major cancer in terms of incidence and mortality in Portugal, and one of the main causes of death due to cancer in both sexes.
The Champalimaud Foundation has made significant efforts in the area of Colorectal Cancer since the launch of its dedicated programme. Ours is a personalised treatment methodology in which the patient is placed at the centre, with the different specialists gravitating around him or her to select the best possible treatment in each individual case.
Digestive Unit
Colorectal Cancer Programme
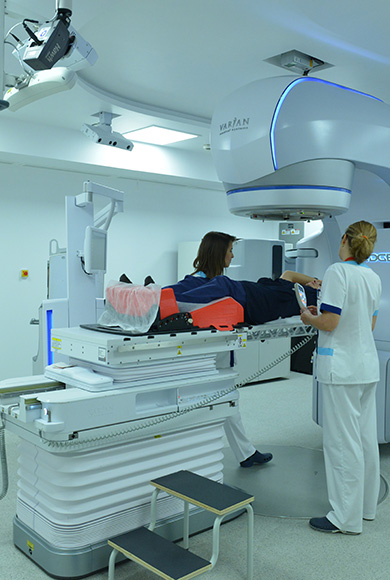
Diagnosis and treatment
The Champalimaud Clinical Centre focuses on delivering integrated oncological care in an efficient way, on facilitating rapid responses that are adequate to the patients’ clinical status, and on the ceaseless search for the best results with the lowest costs. Focused on colon, rectal, oesophageal and stomach tumours, the unit works closely with the Primary and Secondary Liver, Bile Duct and Pancreas Cancer Group and in cooperation with radiologists, pathologists, geneticists, nuclear medicine experts, nurses, psycho-oncologists, nutritionists and palliative care specialists. Prevention and screening of digestive tumours through risk assessment and early cancer diagnosis is of crucial importance in our activity in this area – not only for individual people, but also for the families of patients who have been diagnosed with digestive cancer. This is done mainly through colonoscopy, and through access to the genetic diagnosis services for groups with hereditary risk.
The main targets of this multidisciplinary group of the Digestive Cancer Unit are colon and rectal cancers. At the CCC, we adopt a comprehensive and multidisciplinary approach for the treatment of rectal cancer. This includes advanced forms of radiotherapy, specific rectal imaging techniques and high-precision surgical procedures. We use the most innovative rectal surgery techniques, which together with other treatment options, allow us to achieve high levels of efficacy, minimising the destruction of adjacent healthy tissue and improving patients’ quality of life. Though associated with colon cancer, rectal cancer has been progressively gaining relevance. At the CCC, rectal cancer specialists search, in a multidisciplinary way, for the best forms of treatment, while at the same time working with various scientists in order to develop innovative therapeutic options that can be better tolerated.
In 2014 the Digestive Cancer Unit established an international collaborative programme for the conservative (non-surgical) treatment of rectal cancer, and initiated a treatment and follow-up protocol for these patients. Through this innovative approach, which has been progressively used in various international centres, the Champalimaud Clinical Centre established itself as one of the leading European centres in this area. This recognition has been clearly evidenced through the International Watch and Wait Database, in which the Champalimaud Centre centralises an international registry of over 1,000 patients with rectum conservation following a neoadjuvant treatment based on chemo-radiotherapy.
Digestive Unit
Primary and Secondary Liver, Bile Ducts and Pancreas Cancer Programme
Multidisciplinary, personalised and systematic approach
In the Primary and Secondary Liver, Bile Ducts and Pancreas Cancer Programme we take a multidisciplinary, personalised and systematic approach. We devote ourselves to the diagnosis, treatment and research of primary and secondary (metastases) cancers of the liver, bile ducts and pancreas. This group comprises medical oncologists, pathologists, geneticists, nuclear medicine experts, nurses, psycho-oncologists, nutritionists and palliative care specialists. Such a multidisciplinary approach enables us to draw on different specialties in order to achieve advances in the treatment of cancers that currently have a high mortality rate, such as liver and pancreatic cancers.
The treatment of hepatic metastases has a very important role by allowing an increase in survival rates of patients affected by cancers that tend to only become symptomatic at very advanced stages of the disease. This is what drives our efforts to develop research programmes destined to define new approaches in the characterisation of these lesions and to design news therapeutic modalities based on innovative surgical, radiotherapeutic techniques or other therapeutic modalities (new drugs, radioembolisation, immunotherapy, etc.).
Also of particular relevance is the action developed by the group concerning early diagnosis, given that in these types of cancers, timely detection of the disease significantly increases the available therapeutic options and the capacity to influence control and cure. It was in this context that the Champalimaud Pancreas Programme was created, in order to facilitate the rapid referral of patients with suspicious, solid or cystic pancreatic lesions, and to offer them access to a top-level multidisciplinary medical team, dedicated to the evaluation, study and treatment of pancreatic cysts and carcinomas. The rapid referral system’s ultimate goal is to achieve the best clinical results.

Digestive Unit
Interventional Gastroenterology
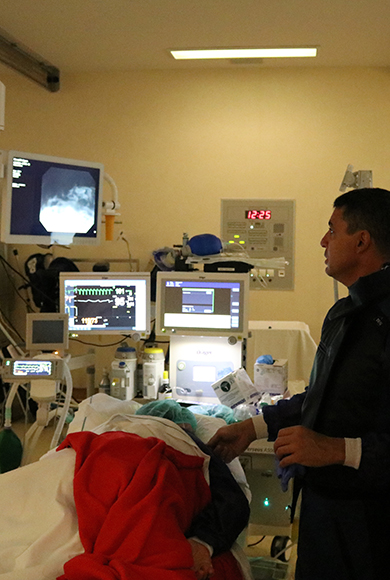
A constantly evolving area
Since 2015, interventional gastroenterology has been utilised at the CCC, with the collaboration of Professor Jacques Devière, of the Université Libre de Bruxelles (Director of the Gastroenterology and Endoscopy Service at Erasmus Hospital). Thanks to his regular presence, the gastroenterology team of the CCC has been developing a diagnostic and endoscopic treatment programme that includes therapeutic techniques such as peroral endoscopic myotomy (POEM) for the treatment of oesophageal motor diseases, and combined approaches of endoscopic retrograde cholangiopancreatography (ERCP) and endoscopy in oncologic pathologies of the bile ducts.


















































